Healthcare / Telehealth
Soaring use of telehealth during crisis driven by deregulation, White House says
By Andrew Sansom | 29 Apr 2020 | 0
The Trump Administration’s deregulatory healthcare agenda has helped spur a jump in telehealth services during the COVID-19 emergency, the White House says, adding that the technology offers many advantages over the long term by increasing healthcare access and providing higher-value care.
Because of advances in smartphones and remote diagnostic testing capabilities, use of telehealth services in the US recently started to increase. But, says the White House, more comprehensive telehealth adoption was held back due in part to issues with internet access, requirements under the Health Insurance Portability and Accountability Act, state licensing laws, provider liability, quality standards, and reimbursement arrangements. A series of deregulatory measures taken by the Federal Government has now been highlighted as a principal reason behind the surge in use of telehealth services during the pandemic.
A few days after the President declared a national emergency, the Centers for Medicare & Medicaid Services (CMS) released guidance on 17 March allowing Medicare to pay for telehealth services provided across the US. And last week, CMS released a new toolkit to help states improve access to the technology among other vulnerable populations through Medicaid.
At the same time as CMS’s Medicare guidance, the HHS Office for Civil Rights announced it would not impose penalties against covered healthcare providers for non-compliance HIPPA rules on privacy and security in connection with the good-faith provision of telehealth. This change allows patients and providers for all types of healthcare to connect over non-public facing video platforms, such as Skype, Zoom and FaceTime, during the national emergency. These policy changes followed a 2018 Department of Veterans Affairs regulation that expanded veterans’ healthcare access to include telehealth and earlier CMS policies to allow virtual check-ins.
The White House points to data showing that telehealth use is increasing because of new flexibilities for the provision of Medicare telehealth services and, potentially, because of HHS’s policy change that allows providers to use popular video platforms to connect with patients. Additionally, the recently enacted Families First Coronavirus Response Act, as amended by the CARES Act, requires group health plans and health insurers to waive cost sharing for COVID-19 testing and any related provider visits to administer such testing, including telehealth visits.
The White House accepts that it is difficult to separate whether the surge in telehealth is primarily driven by patients’ and providers’ shifting preferences due to COVID-19, amendments to or newly enacted legislation, or private insurance reimbursement policies echoing Medicare’s change. But it does suggest that all of these factors have more than likely contributed to telehealth’s growth.
From 14 March to 1 April, daily telehealth claims for upper respiratory infections using ICD-10 diagnosis codes from private insurance increased nearly 12 times from the daily average over the previous month. Upper respiratory infections were chosen for examination because this diagnosis label best represented COVID-19 related illnesses prior to the introduction of a diagnosis code for COVID-19 on 1 April. 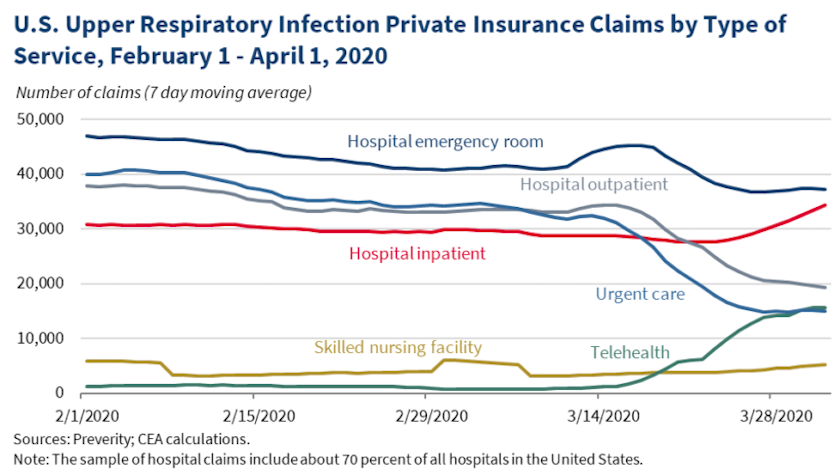
Reduced demand for in-patient care
Telehealth’s recent growth coincides with a significant reduction in use of urgent care and hospital outpatient services since March. Data are not available to clearly demonstrate that patients who would have sought care in urgent care and hospital outpatient departments used telehealth services instead. However, at a time when public health officials are recommending social distancing, telehealth is aligned with this guidance in helping the public avoid crowded healthcare waiting rooms while still getting access to care. Telehealth, says the White House, may also have helped slow the spread of COVID-19 by facilitating social distancing.
Data also show that the use of hospital emergency room and hospital inpatient care for upper respiratory illnesses has remained relatively steady, even with an increase in COVID-19 related upper respiratory illnesses. The Trump Administration says by lowering demand for in-person care, telehealth has helped the healthcare system avoid exceeding capacity during the crisis. Importantly, telehealth can also reduce the negative health outcomes that come from delaying non-COVID-19 care for conditions that require urgent attention, it adds.
Other benefits of telehealth include the potential to expand quality healthcare to individuals with limited access to physical services, including some rural Americans, those who are disabled, and elderly patients who have difficulty travelling. Reduced overhead costs and the overall time it takes to receive accurate diagnoses and treatments are further advantages. All this, says the White House, could see demand for this type continue after the COVID-19 emergency is over.
On 22 April, HHS launched a government portal aimed at providers seeking to deliver telehealth and patients searching for these services. That same day, HHS, through the Health Resources and Services Administration, awarded $150 million to rural hospitals to support, in part, the expansion of telehealth. Another $11.5 million was awarded to 14 telehealth resource centres (TRCs) to provide customised telehealth technical assistance throughout the United States and its territories, while also acting as a clearing house for telehealth research.
While telehealth is likely benefitting public health during the national emergency, the White House underlines that other hypotheses need further analysis so that policymakers can design the most suitable telehealth framework for post-COVID-19 healthcare. Further analyses should examine clinical and insurance data to determine if certain treatments are not appropriate for telehealth and instead require in-person evaluation. Other topics for future evaluation include determining what problems telehealth poses to combating fraud and promoting programme integrity, along with the economic and budget ramifications from increased telehealth use.
Organisations involved

